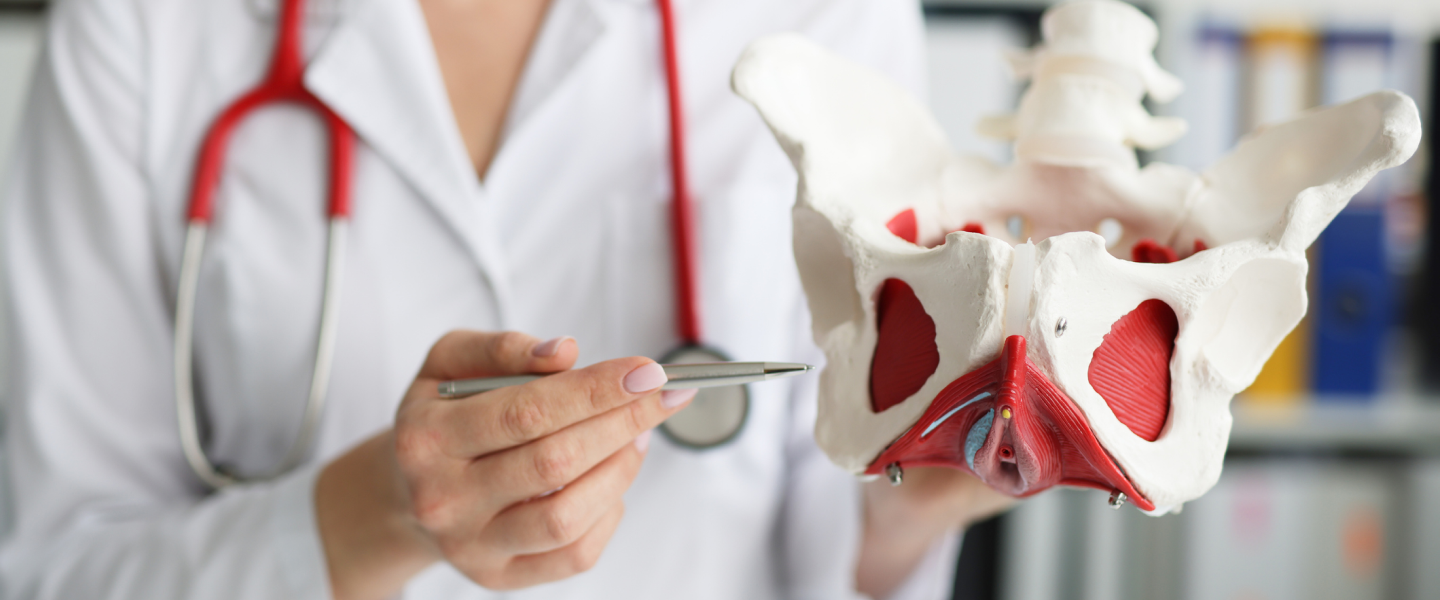
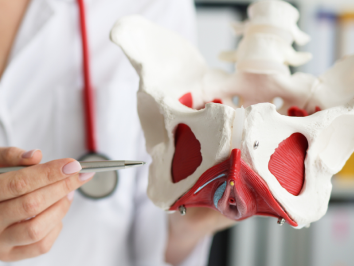
Urogynecology and Reconstructive Pelvic Surgery is one of the rare certification processes approved by two separate Boards: the Board of Obstetrics & Gynecology and the Board of Urology. Rather than dealing with disease, urogynecologists treat conditions that result in abnormal function of the organs within the female pelvic floor.
Restoration of Lost Function
Our goal at EVMS Urogynecology is to restore lost function to our patients, whether pathological, physiological, menopause or prolapse-related. Our treatment options range from physical exercises to medications to reconstructive surgery.
Start the Conversation
One of the hardest discussions a woman will ever have is describing the symptoms of female pelvic floor dysfunction to her doctor. Even though the conversation can be just as embarrassing and uncomfortable as the symptoms themselves, it's important to be as detailed as possible to make sure you receive the correct treatment.
Symptoms (which generally begin gradually and progress with time) can include:
Bladder control problems
- Urine leakage
- Urinary urgency/frequency
- Difficulty emptying the bladder
Pelvic organ prolapse
- A bulging, pressure or a heavy sensation in the vagina that worsens during bowel movements or by the end of the day
Bowel control problems
- Infrequent bowel movement
- Incomplete evacuation of bowels
- Accidental bowel leakage
These symptoms, and any subsequent loss of function, can be effectively diagnosed and treated by competent and skilled physicians like EVMS Urogynecologists Peter Takacs, MD, PhD, MBA, CPE and Kindra Larson, MD, who are both fellowship-trained and board-certified.
Our locations
Urogynecology, Princess Anne
Princess Anne,2075 Glenn Mitchell Drive
Virginia Beach, VA 23456 757.689.5104
Conditions We Treat

Non-surgical Treatments for Urinary Incontinence
There are two predominant types of urinary incontinence: stress incontinence (in which women experience leaking with coughing, sneezing or laughing) and urgency incontinence (a leak with sudden, urgent need to urinate).
Non-surgical treatments include:
- Diet modification
- Medications
- Neuromodulation
- Pelvic floor physical therapy
- Vaginal pessaries

Surgical Options for Urinary Incontinence
Our skilled physicians will discuss all treatment options to help alleviate incontinence.
Surgical options include:
- Botox
- Vaginal slings
- Implantable stimulators
- Urethral bulking
Prolapse
Vaginal prolapse, occurs when the vaginal support weakens and the vagina collapses into the vaginal canal.
Other conditions:
- Interstitial cystitis (bladder pain syndrome)
- Recurrent bladder infections
- Accidental bowel leakage